Dr. Konstantinos Seretis, MD, MSc, EBOPRAS
Assistant Professor
Aesthetic and Reconstructive
Plastic Surgery
Breast Reconstruction
Introduction about Breast Cancer
Risk Factors
Diagnosis
Treatment
Breast Reconstruction
"Life comes with many challenges. The ones that should not scare us are the ones we can take control of."
Angelina Jolie, 1975-
"I look at my cancer journey as a gift: It made me slow down and realise the important things in life and taught me to not sweat the small stuff."
Olivia Newton John, 1948-
BREAST CANCER STATISTICS, 2013-14 *
-
The most common cancer among US women.
-
1 in 8 women in the US will develop invasive breast cancer during their lifetime.
-
29% of newly diagnosed cancers.
-
232.670 new cases will be diagnosed in US.
-
39.620 will die from breast cancer.
-
2.900.000 US women with a history of breast cancer were alive on 1.1.2012.
-
79% of new cases and 88% of breast cancer deaths occurerd in women 50 years of age and older.
-
Half of women who developed breast cancer were 61 years or younger at time of diagnosis (2006 -2010).
-
5-year relative survival is 99% for localized disease, 84% for regional and 24% for distant-stage disease.
-
Breast reconstruction has undergone only 20% of patients after mastectomy.
* American Cancer Society

Recommendations for early breast cancer detection (Screening) *
-
Mammogram every year for women age 40 and older (for as long as they are in good health)
-
Clinical breast exam
-
every 3 years for women 20-40years
-
every year for women above 40years
3. Breast self-exam, for women above 20 years. and report of any breast changes to their doctor.
MRI and Mammogram,every year, for women at high risk (2%), such as:
-
Lifetime risk above 20-25% (based on family history risk assessment tool Claus)
-
Have a known BRCA1, BRCA2 gene mutation.
-
certain high risk factors
-
radiation therapy to the chest between 10-30 years
-
have syndromes Li-Fraumeni, Cowden, Bannayan-Riley-Ruvalcaba or have first-degree relatives with one of these syndromes
-
*American Cancer Society
The breast has a central role in a woman's femininity. Consequently, breast loss, due to breast cancer, is accompanied by a significant psychological impact. Although this is the most common cancer among women, only a small percentage undergoes reconstruction after mastectomy due to a number of myths but also lack of awareness.
We present everything that you need to know, regarding breast cancer and reconstruction after mastectomy.
Risk factors for Breast cancer
A risk factor is anything that affects your chance of getting a disease.
A. Risk factors we cannot change.
-
Gender. Men can develop breast cancer, but this is about 100 times more common among women than men.
-
Aging. The risk increases as someone gets older.
-
Genetic risk factors. About 5% to 10% of breast cancer cases are hereditary (mutations in genes, ig BRCA1, BRCA2). By age 70, 44-78% of women with BRCA1 mutations and 31-56% of BRCA2 mutations will develop breast cancer. These mutations are present in less than 1% of the general population.
-
Family history of breast cancer. Having one first-degree relative (mother, sister, or daughter) with breast cancer approximately doubles a woman's risk. Having 2 first-degree relatives triples the risk.
-
Personal history of breast cancer. A woman with cancer in one breast has a 3- to 4-fold increased risk of developing a new cancer (not a recurrence) in the other breast or in another part of the same breast.
-
Dense breast tissue. Breast is made up of fatty tissue, fibrous tissue, and glandular tissue. Women with more glandular and fibrous tissue have a higher risk of breast cancer.
-
Certain benign breast conditions. Usual conditions such as ductal hyperplasia (without atypia), fibroadenoma, sclerosing adenosis, several papillomas (called papillomatosis) raise a woman's risk slightly (1.5-2 times). Conditions with atypia such as atypical ductal or lobular hyperplasia have a stronger effect on breast cancer risk, raising it 3.5 to 5 times higher than normal.
-
Lobular carcinoma in situ (LCIS). The risk of developing invasive cancer in either breast increases 7- to 11-fold.
-
Number of menstrual periods. Women who have had more menstrual cycles because they started menstruating early (before age 12) and/or went through menopause late (after age 55) have 1-2 times higher risk of breast cancer.
-
Previous chest radiation. The risk varies with the patient's age at time of radiation. The risk is highest if the radiation was given during adolescence. Radiation treatment after age 40 does not seem to increase breast cancer risk.
Β. Risk factors we can change
-
Having children. Women who have had no children or who had their first child after age 30 have 1-2 times higher breast cancer risk.
-
Recent use of contraceptives. The risk increases 1-2 times, but women who stopped using oral contraceptives more than 10 years ago do not appear to have any increased breast cancer risk.
-
Hormone therapy after menopause. There are 2 types:
-
Combined hormone therapy. The increase in risk can be seen with as little as 2 years of use. The risk increases only to current and recent users and returns to that of the general population within 5 years of stopping them.
-
Estrogen therapy. The breast cancer risk is not increased. However, the risk of strokes, blood clots and ovarian cancer (when used for more than 10 years) is increased.
-
-
Breastfeeding. Some studies suggest that breastfeeding may slightly lower breast cancer risk, especially if it is continued for more than a year.
-
Alcohol. The risk increases with the amount of alcohol consumed.
-
Being overweight or obese, after menopause. The risk increases.
-
Physical activity. Brisk walking, as little as 1.25 to 2.5 hours per week, reduced a woman's risk by 18% in a recent study.
The influence of several other factors is under study, with results either inconclusive or negative. Factors such as diet and vitamin intake, chemicals, tobacco smoke and night work have been studied with inconclusive findings. Factors such as the use of bra, antiperspirants, spontaneous induced abortion and breast implants do not increase the risk of breast cancer, according to the existing data.
Diagnosis
Breast cancer is diagnosed either due to symptoms or after screening tests. This is why getting the recommended screening tests is so important. An early diagnosis is usually done before clinical signs and thus the cancer is treated better, with higher success rates.
The most common symptom of breast cancer is a new lump or mass. A painless, hard mass that has irregular edges is more likely to be cancerous, but breast cancers can be also appeared tender, soft, or rounded. They can even be painful. For this reason, it is important to have any new breast mass, lump or breast change checked by a doctor.
Other possible signs of breast cancer include:
-
Swelling of all or part of a breast (even if no distinct lump is felt)
-
Skin irritation or dimpling
-
Breast or nipple pain
-
Nipple retraction (turning inward)
-
Redness, scaliness or thickening of the nipple or breast skin
-
Nipple discharge (other than breast milk)
-
A lump or swelling in the axilla or below the collar bone (even before the original tumor in the breast can be felt)
Although any of these symptoms can be caused by conditions other than breast cancer, they should be reported to a doctor for further examination. Your doctor will take a history, will examine you and probably send you for further testing before any definite diagnosis can be done.
Treatment
The treatment of breast cancer is surgical in order to remove the tumor. The operation differs according to the cancer stage. Similarly, further treatment such as radiation therapy,chemotherapy, hormone therapy and targeted therapy (monoclonal antibodies) may be required.
Surgical options include breast-conserving surgery and mastectomy:
-
Breast conserving surgery. It only removes a part of the affected breast, which depends on the size and location of the tumor (and other factors). For most women with stage I or II breast cancer, breast-conserving surgery (BCS) plus radiation therapy is as effective as mastectomy. Survival rates of women treated with these 2 approaches are the same.
-
Mastectomy. There are the following types:
-
Total or simple mastectomy, the entire breast is removed, including the nipple.
-
Skin sparing mastectomy. the entire breast tissue is removed, but the skin over the breast (other than the nipple and areola) is left intact. This approach is only used when immediate breast reconstruction is planned.
-
Nipple sparing mastectomy, the breast tissue is removed, but the breast skin and nipple are left in place. This is followed by breast reconstruction. Although technical improvements have made it safer, many experts consider nipple-sparing procedures too risky to be a standard treatment of breast cancer.
-
Modified radical mastectomy. This procedure is a simple mastectomy together with removal of axillary lymph nodes. It is indicated in more advanced stages of the disease.
-
Radical mastectomy. The entire breast, axillary lymph nodes, and the pectoral muscles are removed. Currently, this operation may still be done for large tumors of the pectoral muscles (under the breast).
Choosing the best surgical option is based on multiple factors, which is beyond the informative purpose of this site. Your breast surgeon will inform you about the available options, which fit to your case, as each case is different.

Breast Reconstruction
Breast reconstruction is a type of surgery for women who have had all or part of a breast removed. The surgery rebuilds the breast mound so that it is about the same size and shape as it was before. The nipple and the darker area around the nipple (areola) can also be added. Most women who have had a breast removed (mastectomy) can have reconstruction. Breast reconstruction is done by a plastic surgeon.
A Plastic Surgeon is responsible to inform you regarding the reconstructive options, plan and perform the operation. We suggest to discuss the best available options for your case after the breast cancer diagnosis and before the mastectomy. Your case is thoroughly analyzed and the treatment plan is organized. The knowledge that your breast will be reconstructed, either immediately or delayed, improve your psychology before the mastectomy.
Unfortunately, only a minority of mastectomy patients have a breast reconstruction.
Why have breast reconstruction?
Women choose breast reconstruction for many reasons:
-
To permanently regain their breast shape
-
To make their chest look balanced when they are wearing a bra or swimsuit
-
To improve their body image, self-esteem and their quality of life
Breast reconstruction can not built a breast exactly the same with the normal breast, because the tissue characteristics are different. You will be able to see the difference between the reconstructed breast and the remaining breast when you are nude. But when you’re wearing a bra, the breasts should be alike enough in size and shape that you’ll feel comfortable about how you look in most types of clothes. Your body image and self-esteem may improve after your reconstruction surgery, but this is not always the case. Some women are not happy with how the reconstructed breast looks and feels after surgery, and there may be concerns about the flap or donor sites too.
You and those close to you must know what to expect from reconstruction. There are often many options to think about as you and your Plastic Surgeon talk about what’s best for you. The reconstruction process often means one or more operations. Talk about the benefits and risks of reconstruction with your doctors before the surgery is planned. Give yourself plenty of time to make the best decision for you. You should make your decision about breast reconstruction only after you are fully informed.
Immediate or Delayed breast reconstruction?
Immediate breast reconstruction is done, or at least started, at the same time as the mastectomy.
Advantages:
-
Less surgery (2 operations in 1 are done)
-
Less scaring (tissues are not damaged by radiation or surgery)
-
Better, usually, aesthetic outcome
-
No breast loss at all (which has also psychological impact)
Disadvantages:
-
requires more surgical and anaesthetic time
-
higher risk of complications (due to combination of operations)
-
potential complications may delay further treatment, which is required
-
potential radiotherapy, after the reconstruction, may affect the outcome
-
requires availability of both breast and plastic surgeon
The option of immediate reconstruction is not always feasible and depends on many factors such as the stage of breast cancer, woman's health, need for radiotherapy etc. Smoking is absolute contraindication for immediate reconstruction due to increased risk of skin necrosis. Moreover, some women do not want to think about reconstruction while coping with a diagnosis of cancer. If this is the case, you might choose to wait until after your breast cancer surgery to decide about reconstruction.
Delayed breast reconstruction means that the rebuilding starts later, after mastectomy and potential further treatment has been completed.
Advantages:
-
treatment for cancer has been completed
-
tissues have healed, so the risk of skin necrosis is reduced
-
damaged tissue from radiotherapy may be reconstructed
Disadvantages:
-
need for a second, at least, operation
-
need for postoperative recovery time
-
scars from previous mastectomy may affect the final outcome
Delayed breast reconstruction is associated with very high satisfaction rates and improved quality of life, as it is recorded from various medical studies. Every operation has its indications, and thus a thorough discussion with the Plastic Surgeon will illustrate the aspects of the breast reconstruction.
Breast implants or autologous tissues?
Α. The Breast implants are silicone gel-filled implants (like in breast augmentation), with a preference in anatomical implants, because they provide a more natural result. Available types of implant surgery:
-
One-stage immediate breast reconstruction. After the breast surgeon removes the breast, a plastic surgeon places a breast implant, beneath the pectoral muscle. The technique is similar in concept to breast augmentation but very different from the technical point of view, as no breast exists. The special implant features and the potential use of other materials are othe rimportant differences.
-
Two-stage delayed reconstruction is the type most often done if implants are used. An implanted tissue expander (like a balloon), is put under the skin and chest muscle. Through a tiny valve under the skin, the Plastic Surgeon injects a salt-water solution at regular intervals to fill the expander. After 4-6 months, the skin over the breast area has stretched enough, so a second surgery will remove the expander and put in the permanent breast implant.
-
Delayed-immediate reconstruction, in two stages. It is used when the patient wants immediate reconstruction but the treatment plan is ambiguous due to the cancer features. A temporary expander implant is used just after mastectomy, so the woman has immediately a breast mound but the reconstruction is not completed before the biopsy results and potential further treatment.
The implant-based breast reconstruction has advantages, such as:
-
short operation time
-
limited pain and risk of immediate complications
-
no donor tissue from patient body is used
-
great results when they are used for prophylactic mastectomy (Angelina Jolie case)
Disadvantages are:
-
risk of immediate complications, such as after any operation (bleeding, hematoma, infection, delayed wound healing, hypertrophic scar etc)
-
risk of late complications from the implant such as rupture, fluid collection (seroma), infection, capsular contractures that may require further treatment
-
risk of implant removal or exchange in the first 10 years after reconstruction. This risk is much higher than the aesthetic breast augmentation
-
need for further operation to complete the reconstruction
-
result is not very natural, as the breast does not change in size as you gain or lose weight, is immobile and colder than the normal breast. An operation on the normal breast may be required for a better symmetry to be achieved
-
poor result in women with large ptotic breasts
-
need for MRI test to check implant status
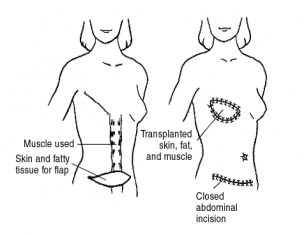
Β. Autologous tissues (flaps). Usual donor areas are the abdomen (TRAM or DIEP flap) and the upper back (Latissimus Dorsi flap) of the patient. Skin together with fat and possibly muscle (rectus abdominis, latissimus dorsi) is taken to create the breast.
TRAM DIEP Latissimus Dorsi
flap flap flap
Advantages are:
-
The tissue composition of flap is similar to the natural breast, because of the amount of fat
-
the breast behaves more like the rest of the body tissue,as it moves, changes in size and has the body temperature. The need to operate on the other breast is also less but still possible, because of ptosis, size etc.
-
avoid an implant use and thus potential complilcations
-
good result in women with large ptotic breast
-
use of a flap from the abdomen offers an abdominoplasty at the same time
Disadvantages are:
-
tissue from the patient is used so it leaves 2 surgical sites and thus scars
-
long operation time, which varies and may reach 10-12 hours (DIEP flap)
-
longer recovery time
-
risk (5-10%) of total flap necrosis, mainly with use of flaps with microsurgical technique (DIEP flap)
-
insufficient flap tissue in very slim patients
-
the use of abdominal muscle (TRAM flap), reduces the power of the abdomen, which may cause a hernia
Breast reconstruction with autologous tissues is advised in most cases despite of potential complications. Many factors should be considered like the patient's health, body type, desires, tissue availability, smoking, etc. The discussion with the Plastic Surgeon will assist you to decide the best option for you.
After breast reconstruction surgery?
The breast reconstruction is completed with:
-
Reconstruction of nipple areola complex. This is an aesthetic reconstruction with the use of a nipple graft from the normal breast or a local flap. The areola is reconstructed with a skin graft and/or medical tattoo.
-
Symmetrization operation on the normal breast, with the use of a type of mastoplasty (augmentation, reduction or mastopexy)
-
Fat grafting is a new option in order to correct volume deficiency, breast asymmetry or minor irregularities.
Although these operations are not always necessary to be done, they improve considerably the aesthetic outcome and thus the patient satisfaction from the reconstruction process.
In conclusion, breast reconstruction after mastectomy is a process where patient awareness has a central role in choosing the technique which will fulfill her needs. The trust, discussion and cooperation with your Plastic Surgeon is necessary in order to complete successfully the treatment of cancer and breast reconstruction process.